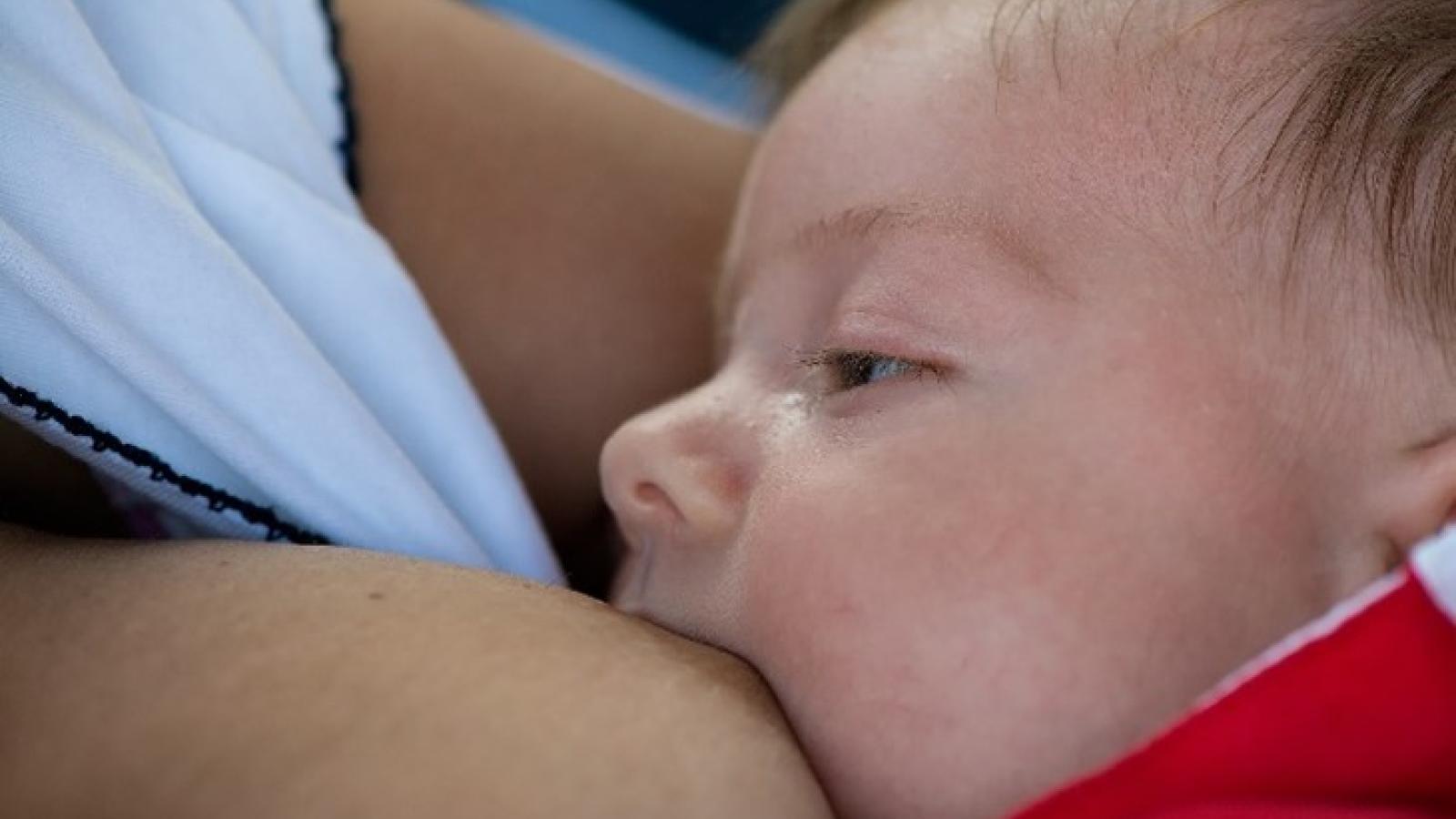
Your breast milk is perfect and unique for your baby. It gives them all the nutrition they need, for the first six months of their life.
From six months, you can introduce solid food to your baby, alongside breastfeeding. Ideally, if you can, continue breastfeeding for up to 2 years or more.
On this page:
Benefits of breastfeeding
- Helps build a strong emotional bond and attachment between you and your baby. This helps your baby feel safe and secure.
- Breast milk helps to protect your baby from infections and diseases. It will provide long-term health benefits into adulthood. Breastfeeding will reduce allergies, asthma, digestive problems, and obesity.
- Is a fantastic opportunity for skin-to-skin contact. Your body releases positive hormones when strengthening your bond with your baby.
- Provides time to gaze at each other and opportunities to communicate. You will both speak, through eye contact and facial expression.
- Provides time to connect with each other in a close and intimate way.
- Is always available so allows you to be responsive to your baby whenever they show you that they need to be fed.
- Can reduce your risks of future diseases, including:
- Breast and ovarian cancer
- Osteoporosis (weak bones)
- Cardiovascular disease
- Obesity
- Dementia
- Breast milk is all your baby will need for the first 6 months (there is no need to give your baby water in hot weather). Your milk will adapt to the needs of your baby. NHS Start for Life has more helpful information.
Responding to your baby’s cues

Breastfeeding involves you responding to your baby’s cues, as well as your own need to feed your baby. Feeds are more than nutrition. They're also for love, comfort, and reassurance between you and your baby.
It is important to understand how to respond to your baby’s cues when they are hungry. Crying is the last sign of wanting to feed, so try and feed before your baby cries.
Signs that your baby is hungry could be:
-
Licking or smacking their lips, opening their mouth, turning their head
-
Chewing their fist, stretching, wriggling
You can offer your baby the breast whenever you wish to, not just when they are hungry. There are many reasons for both you and your baby why it might feel right to feed including:
-
To calm your baby if they are unsettled
-
Following immunisations or if they are unwell
-
If you or your baby are in an unfamiliar environment
-
Before you go out and before bedtime
-
If you need a rest, a sit-down, or some quiet time with your baby
-
Because your instincts tell you
-
To ease full breasts
UNICEF has an information sheet you can download called Responsive Feeding.
Positioning: How to breastfeed your baby
There are many different positions to feed your baby and you will find what works best for you and your baby. Try to:
- Create as calm an environment for yourself as possible
- Have a drink of water and food for yourself nearby
- Try and relax your shoulders and support your arms
- Be comfortable
When your baby is ready to feed, hold them close with no blankets or little arms between you. Your baby needs to be able to tip their head back to get a big mouthful of breast. Support your baby around the base of their neck and shoulders rather than their head.
Start with your baby’s nose opposite your nipple rather than their mouth. This will allow your baby to reach up, tip their head back and attach to the breast. Your baby should have a large mouthful of breast. Your nipple should be drawn back to the soft palate (the back) of your baby’s mouth.
If your baby is not attached deeply enough this could become painful for you and your baby may not get enough milk.
Laid back breastfeeding
Laid back breastfeeding can be an effective and comfortable way of feeding your baby. All you need to do is recline - as much or as little as is possible or as you want to.
Laid back breastfeeding encourages your baby’s natural breastfeeding instincts.
When you lean back, your body supports your baby’s weight which leaves you more hands-free. It takes the pressure off your back, neck, and shoulders.
- Put your baby to your chest, gravity will keep your baby in position
- Make sure your head and shoulders are well supported. Let your baby’s whole front touch your whole front
- As you are leaning back, your baby will not be able to sit in your lap. Let your baby rest on you in any position, making sure their whole front is against yours. Let your baby’s cheek rest somewhere near your bare breast
- Help your baby to find your breast and relax and enjoy the feed
UNICEF's 'Off to the best start' leaflet gives you more information.
Expressing milk
If you do not need to express milk, it's best to wait until your baby and you feel confident with breastfeeding. Waiting until your baby is around 4-6 weeks will enable your milk flow to establish.
Expressing breast milk, if your baby is unwell, or premature can help them. Your baby will get all the nutrients they need and protection against infection.
It also means that you can build your milk supply ready for when your baby is able to feed at the breast.
You may choose to express milk so that a co-parent can become involved in feeding your baby. Or if you must return to work or study, expressing can help you continue breastfeeding.
It's a good idea to chat this over with someone before you start.
When your milk first arrives, from day 3 you may need to relieve your breasts of some milk to enable your baby to attach. Hand expressing can help with this.
There are different ways you can express your milk:
- Hand expressing
- A manual pump
- An electric pump
If you're expressing because you're back at work or study, these links may help:
Storing breast milk
You can safely store expressed breast milk at home if:
- In a sterile container with a lid.
- In a sealed container at room temperature for up to 6 hours.
- Placed and stored at the back and bottom of a fridge for up to 5 days if the fridge is at 4˚C or lower.
- Stored in the ice compartment of a fridge for up to 2 weeks
- Stored in a deep freeze for up to 6 months if freezer at -18˚C or lower.
Before using expressed breastmilk, you may notice the milk separates. Gently swirling the milk will help mix the contents.
Frozen milk will need to be defrosted in the fridge overnight and used within 12 hours. Never refreeze frozen milk, once thawed. You may warm the milk to body temperature by standing the milk in warm water. Do not heat in a microwave.
For more information, see The Breastfeeding Network's leaflet Expressing and Storing Breastmilk.
Breastfeeding challenges
There may be times when breastfeeding can be challenging and some common worries are:
Milk supply
The more you feed your baby the more milk you will produce. Your baby will show signs that they are getting enough. Your baby will be relaxed and calm during and after a feed and they come off the breast by themselves. Talk through any concerns with your healthcare professional or a breastfeeding supporter.
Useful articles to read:
- Low milk supply 101 from the Association Breastfeeding Mothers
- Breastfeeding: is my baby getting enough milk? from NHS
Your baby will breastfeed more at night and this can be exhausting. Try and sleep when your baby does in the early days. These night-time feeds between 2am and 5am will help to increase your milk supply.
Your baby should have lots of wet and dirty nappies every day. This is one of the best signs that they are getting enough milk. For more information, see Newborn baby poo in nappies: what to expect from National Childbirth Trust (NCT).
Your health visitor or GP will guide you if your baby isn't gaining weight. (See below for national support options).
Mastitis
This is when the breast tissue becomes inflamed and painful. You may also feel tired and have flu like symptoms. Although it is painful it is important to try and continue to breastfeed or express as usual. There are lots of self-help measures you can take. You will need to make an appointment with your GP if:
- Symptoms continue for more than 24 hours
- You feel very unwell
There's more information in the Breastfeeding Network leaflet: Mastitis and breastfeeding.
Nipple soreness and sensitivity
Soreness can be common in the early weeks of breastfeeding. It will happen if your baby is not latching on properly. See our section on positioning to help. The NHS Start for Life website also has further information on sore nipples.
Tongue-tie
This can prevent your baby from latching on properly and can also be a cause of sore or cracked nipples. It is when the strip of tissue that attaches your baby’s tongue to the base of their mouth is shorter than usual.
If you're worried that your baby may have tongue-tie, contact your midwife, health visitor or GP. NHS Start for Life also has further information on tongue-tie.
Crying
Babies and children will cry. ICON Parents Advice provides information explaining:
- Infant crying is normal
- Comforting methods can help
- It’s OK to walk away
- Never, ever shake a baby
For local support available, ask your midwife or health visitor for details.
Breastfeeding helplines and websites
There is lots of advice and guidance out there to help you:
NHS
- Your breastfeeding questions answered
- Benefits of breastfeeding
- Start for Life breastfeeding help and support
- There is also advice on bottle feeding and mixed feeding so you can make informed choices using clear NHS impartial information.
- Breastfeeding Friend support service: Available 24/7, 365 days a year on Amazon Alexa, Google Home, and Facebook Messenger. Access to NHS advice – based on questions asked by thousands of new mums – and daily tips.
- Sign up for email advice: regular email with tips and advice on pregnancy, baby, and parenting.
- Chestfeeding if you're trans or non-binary
National Breastfeeding Helpline: Confidential breastfeeding information and support. Lines are open 9:30am to 9:30pm, 365 days a year. Support is also available in Welsh, Polish, Bengali & Sylheti and for people who have hearing or speech impairments.
The Breastfeeding Network: Breastfeeding support and information.
Association of Breastfeeding Mothers
La Leche League: Mother-to-mother support with breastfeeding.
National Childbirth Trust (NCT): Information and support on all aspects of pregnancy, birth, and early parenthood, including breastfeeding.
The Twins Trust: Information about feeding twins and triplets.
Drugs in Breast Milk Help
- Get support via email: [email protected] or Facebook
Lactation Consultants of Great Britain: Help you find a lactation consultant near you.
UK Association of Milk Banking: Information about using donated breast milk if your baby is premature or ill, and how to donate breast milk.
UNICEF UK Baby Friendly Initiative
Healthy Mom & Baby: Lactation Options & Strategies for LBGTQ Persons
La Leche League: Support for Transgender & Non-binary Parents